A study of risk factors for patients with Diabetic foot ulcer
Abstract
Background: Peripheral neuropathy and peripheral vascular diseases are the important causes of non-traumatic lower limb amputation. The risk of amputation among diabetic patients increases by two to four folds with the advancement of age and duration of diabetes.It has also been proven by many longitudinal epidemiological studies that among diabetic patients, the life time foot ulcer risk is about 25%, thereby accounting for two thirds of all non-traumatic amputations. Clinical guidelines recommend that all patients with diabetes should be screened annually to establish their risk of foot ulceration.
Aim: To ascertain the risk factors leading to amputation for patients with diabetic foot ulcer.
Materials and method: The present study was conducted in the Department of General Surgery of Melmaruvathur Adhiparasakthi institute of medical sciences. Melmaruvathur. For our study, we selected 200 patients admitted to the surgical ward with diagnosis of diabetic foot ulcer. History of diabetic status of patient, whether patient was a undetected case or a known diabetic, if known the duration of the disease, whether patient was on regular or irregular treatment (diet/oral/drugs/insulin) were recorded. Lab tests of each patient were conducted for hemoglobin, TLC, DLC, ESR, blood urea, serum creatinine and blood sugar. All the cases were managed following conservative and surgical approach.
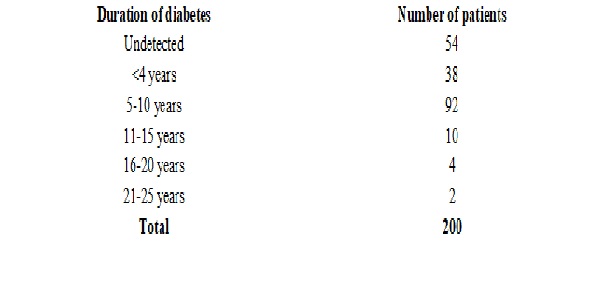
Results: A total of 200 patients were present in the study group. The mean of the subjects was 49.28 + 6.88 years. Out of 200 patients, 46 were females and 154 were males. We observed that 54 patients were undetected at the time of admission at hospital. Majority of patients (n=46) had duration of diabetes from 5-10 years. 38 patients had duration of diabetes less than 4 years, 10 patients had duration of diabetes from 11-15 years. Most of the patients present with more than one lesion. Only major lesion is considered here. Ulcer was the major lesion seen in present series being present in 144 patients.
Conclusion: We conclude that Routine foot care should be available to every patient with diabetes ideally, but the reality of most of these patient slack adequate knowledge and resources resulting in the absence of such care.
Downloads
References
2. Pecoraro RE, Reiber GE, Burgess EM. Pathways to diabetic limb amputation. Basis for prevention. Diabetes Care. 1990 May;13(5):513-21.[pubmed]
3. Adler AI, Boyko EJ, Ahroni JH, Smith DG. Lower-extremity amputation in diabetes. The independent effects of peripheral vascular disease, sensory neuropathy, and foot ulcers. Diabetes Care. 1999;22:1029–35. doi: 10.2337/diacare.22.7.1029.
4. Lehto S, Rönnemaa T, Pyörälä K, Laakso M. Risk factors predicting lower extremity amputations in patients with NIDDM. Diabetes Care. 1996;19:607–12. doi: 10.2337/diacare.19.6.607.
5. Trautner C, Haastert B, Giani G, et al. Incidence of lower limb amputations and diabetes. Diabetes Care. 1996 Sep;19(9):1006-9.[pubmed]
6. Siitonen O, Niskanen L, Laakso M, Siitonen J, Pyorala K. Lower-extremity amputations in diabetic and nondiabetic patients. A population-based study in eastern Finland. Diabetes Care. 1993;16:16–20. doi: 10.2337/diacare.16.1.16.
7. Unwin N. Epidemiology of lower extremity amputation in centres in Europe, North America and East Asia DOI:10.1046/j.1365-2168.2000.01344.x
8. International Working Group on the Diabetic Foot. Epidemiology of Diabetic Foot Infections in a Population Based Cohort. Noordwijkerhout, The Netherlands; 2003.
9. Lavery LA, Armstrong DG, Wunderlich RP, et al. Diabetic foot syndrome: evaluating the prevalence and incidence of foot pathology in Mexican Americans and non-Hispanic whites from a diabetes disease management cohort. Diabetes Care. 2003 May;26(5):1435-8.[pubmed]
10. Boulton AJ, Vileikyte L, Ragnarson-Tennvall G, et al. The global burden of diabetic foot disease. Lancet. 2005 Nov 12;366(9498):1719-24.DOI:10.1016/S0140-6736(05)67698-2.[pubmed]
11. Shahbazian H, Yazdanpanah L, Latifi SM. Risk assessment of patients with diabetes for foot ulcers according to risk classification consensus of International Working Group on Diabetic Foot (IWGDF). Pak J Med Sci. 2013 May;29(3):730-4.[pubmed]
12. Wu L, Hou Q, Zhou Q, et al. Prevalence of risk factors for diabetic foot complications in a Chinese tertiary hospital. Int J Clin Exp Med. 2015 Mar 15;8(3):3785-92. eCollection 2015.[pubmed]
13. Sarinnapakorn V, Sunthorntepwarakul T, Deerochanawong C, et al. Prevalence of Diabetic Foot Ulcers and Risk Classifications in Type 2 Diabetes Mellitus Patients at Rajavithi Hospital. J Med Assoc Thai. 2016 Feb;99 Suppl 2:S99-105.[pubmed]
14. Nyamu PN, Otieno CF, Amayo EO, et al. Risk factors and prevalence of diabetic foot ulcers at Kenyatta National Hospital, Nairobi. East Afr Med J. 2003 Jan;80(1):36-43.[pubmed]


 OAI - Open Archives Initiative
OAI - Open Archives Initiative


















 Therapoid
Therapoid

