Rational use of antibiotics and its guidelines in surgical patients-a retropspective study
Abstract
Introduction: Rational use of drugs means to prescribe the appropriate drugs in correct dose over an adequate period of time at a lower cost. Irrational use of antibiotic is harmful both for the patient and the society and hence the top cause of mortality and morbidity around the world. So the aim of the present study is to - 1. Avoid adverse effect of irrational use of antibiotics on patient. 2. Avoid emergence of antibiotic resistance. 3. Avoid unnecessary increase of cost of health care.
Methods: The study was conducted at the Surgery Unit II of the ESI-PGIMSR and ESIC Medical College, Joka, Kolkata- 700104, West Bengal. The Data was collected on random basis and the SSI was observed between the control and test group after rational and non rational treatment with antibiotics in some selected surgical patient.
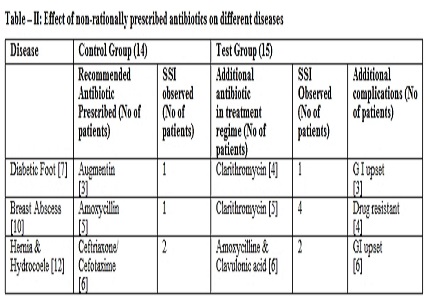
Results: It was found that in some diseases like acute gall bladder stone, cholecystitis, appendicitis, pancreatitis if some other antibiotics are additionally used besides the recommended as usual antibiotics the significant betterment is achieved in relation to quick recovery of the patients along with minimization of surgical site infection with no other complications. On the other hand in some other diseases like Diabetes foot, hernia, etc. use of antibiotics beyond the recommended antibiotics aggravates some other complications in the patients along with no significant betterment of surgical site infection in Test group.
Conclusion: To conclude finally antibiotic resistance is a major problem worldwide and is inevitable and hence its rational use in proper guidelines is the only way of prolonging the useful life of the patients requiring antibiotics.
Downloads
References
2. Kotwani A, Holloway K, Chaudhury RR. Methodology for surveillance of antimicrobials use among out-patients in Delhi. Indian J Med Res. 2009 May;129(5):555-60.
3. Mathew JL. Pneumococcal vaccination in developing countries: where does science end and commerce begin? Vaccine. 2009;27:4247–51.
4. Austin DJ, Kristinsson KG, Anderson RM. The relationship between the volume of antimicrobial consumption in human communities and the frequency of resistance. Proc Natl Acad Sci U S A. 1999 Feb 2;96(3):1152-6.
5. Laxminarayan R, Malani A, Howard D, Smith D. Washington, DC: 2007. [updated 2007; cited]. Policy responses to the growing threat of antibiotic resistance.
6. Goossens H. Antibiotic consumption and link to resistance. Clin Microbiol Infect. 2009 Apr;15 Suppl 3:12-5. doi: 10.1111/j.1469-0691.2009.02725.x. [PubMed]
7. Apisarnthanarak A, Mundy LM. Correlation of antibiotic use and antimicrobial resistance in Pratumthani, Thailand, 2000 to 2006. Am J Infect Control. 2008 Nov;36(9):681-2. doi: 10.1016/j.ajic.2007.10.022.
8. Albrich WC, Monnet DL, Harbarth S. Antibiotic selection pressure and resistance in Streptococcus pneumoniae and Streptococcus pyogenes. Emerg Infect Dis. 2004 Mar;10(3):514-7. [PubMed]
9. Chokejindachai W. Current situation of antimicrobial resistance in Thailand: a review. Nonthaburi: Health System Research Institute; 2007.
10. Jitraknatee A. Antibiotic values. In: Niyada Kiatying-Angsulee, Nusaraporn Kessomboon, Usawadee Maleewong, editors. Situation report on drug system 2010: antimicrobial resistance. Bangkok: Drug System Monitoring and Development Center; 2011.
11. Bhavnani D, Phatinawin L, Chantra S, Olsen SJ, Simmerman JM. The influence of rapid influenza diagnostic testing on antibiotic prescribing patterns in rural Thailand. Int J Infect Dis. 2007 Jul;11(4):355-9. Epub 2007 Feb 26.
12. Suttajit S, Wagner AK, Tantipidoke R, Ross-Degnan D, Sitthi-amorn C. Patterns, appropriateness, and predictors of antimicrobial prescribing for adults with upper respiratory infections in urban slum communities of Bangkok. Southeast Asian J Trop Med Public Health 2005; 36: 489-97.
13. Udomthavornsuk B, Tatsanavivat P, Patjanasoontorn B, Khomthong R, Bhuripanyo K, Saengnipanthkul S, Lumbiganon P, Wiengnond S, Boonma P, Vongsangnak V, et al. Intervention of inappropriate antibiotic use at a university teaching hospital. J Med Assoc Thai. 1991 Oct;74(10):429-36.
14. Pagaiya N, Garner P. Primary care nurses using guidelines in Thailand: a randomized controlled trial. Trop Med Int Health 2005; 10: 471-7 doi: 10.1111/j.1365-3156.2005.01404.x.
15. Earnshaw S, Monnet DL, Duncan B, O'Toole J, Ekdahl K, Goossens H; European Antibiotic Awareness Day Technical Advisory Committee; European Antibiotic Awareness Day Collaborative Group. European Antibiotic Awareness Day, 2008 - the first Europe-wide public information campaign on prudent antibiotic use: methods and survey of activities in participating countries. Euro Surveill. 2009 Jul 30;14(30):19280.
16. Selecteddrug used indicator World Health Organization 1 Academic Press (1998). The World Medicins Situation20.
17. Swindell PJ, Reeves DS, Bullock DW, Davies AJ, Spence CE. Audits of antibiotic prescribing in a Bristol hospital. Br Med J (Clin Res Ed). 1983 Jan 8;286(6359):118-22. [PubMed]
18. Gonzales R, Steiner JF, Sande MA. Antibiotic prescribing for adults with colds, upper respiratory tract infections, and bronchitis by ambulatory care physicians. JAMA. 1997 Sep 17;278(11):901-4. [PubMed]


 OAI - Open Archives Initiative
OAI - Open Archives Initiative


















 Therapoid
Therapoid

