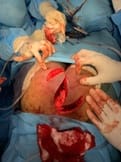
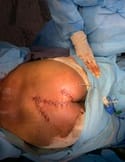
A Comparative Study on flap necrosis following Karydakis Flap Reconstruction and Z-Plasty in Patients with Sacrococcygeal Pilonidal Disease – Our experience
Gayathre S.1, Kumar R.2*, Prabu M.3, R Kannan M.S.4
DOI: https://doi.org/10.17511/ijoso.2021.i04.02
1 SP Gayathre, D.G.O., M.S, Professor, Institute of General Surgery, Madras Medical College, Chennai, Tamilnadu, India.
2* R Niranjan Kumar, M.S Gen surgery, D.Ortho, Institute of General Surgery, MMC, Chennai, Tamilnadu, India.
3 MJ Prabu, MBBS., Postgraduate (General surgery), Institute of General Surgery, MMC, Chennai, Tamilnadu, India.
4 R Kannan M.S., Professor and Head of the department, Institute of General Surgery, Madras medical college, Chennai, Tamilnadu, India.
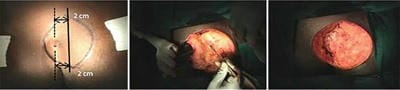
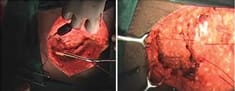
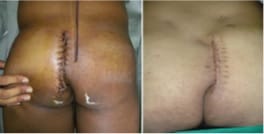
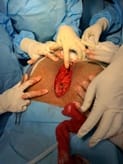
Aim: The purpose of this study was to evaluate patients with sacrococcygeal pilonidal sinus disease (SPSD) who underwent the Karydakis procedure and Z plasty at our centre concerning the perioperative findings, late postoperative results and recurrence. Patients and Methods: A total of 30 patients presenting with SPSD at our centre underwent Karydakis flap repair and Z plasty from May 2019 to June 2021. These patients were then followed up and evaluated concerning operative time, drain use, hospital stay, suture removal, complications, and recurrence. The adipocutaneous flap of Karydakis was devised to shift the natal cleft, while Z-plasty involves a fasciocutaneous flap. Results: The mean operative time was 60 min with a median hospital stay of 4 days. Drains were removed at a median of 5 days and sutures at a median of 15 days. The duration of hospitalisation for the Karydakis procedure was found significantly lesser than that for Z-plasty Patients who were followed up for a median of 12 months. The overall complications were more in Z-plasty. Flap necrosis developed in 30 % of the cases in the Z-plasty group, comparable to no recurrence seen in the Karydakis procedure. Conclusion: Karydakis flap was found superior to Z-plasty, having less seroma formation, no flap necrosis and no local hematoma Karydakis flap procedure is a relatively simple procedure for SPSD and has advantages over Z-plasty technique like keeping scar away from the midline and flattening of the natal cleft, thus reducing local recurrence rates.
Keywords: Complications, Karydakis flap repair, Z-plasty technique, Pilonidal sinus recurrence
| Corresponding Author | How to Cite this Article | To Browse |
|---|---|---|
| , M.S Gen surgery, D.Ortho, Institute of General Surgery, MMC, Chennai, Tamilnadu, India. Email: |
SP Gayathre, R Niranjan Kumar, MJ Prabu, R Kannan M.S., A Comparative Study on flap necrosis following Karydakis Flap Reconstruction and Z-Plasty in Patients with Sacrococcygeal Pilonidal Disease – Our experience. Surgical Rev Int J Surg Trauma Orthoped. 2021;7(4):85-90. Available From https://surgical.medresearch.in/index.php/ijoso/article/view/240 |


 ©
©